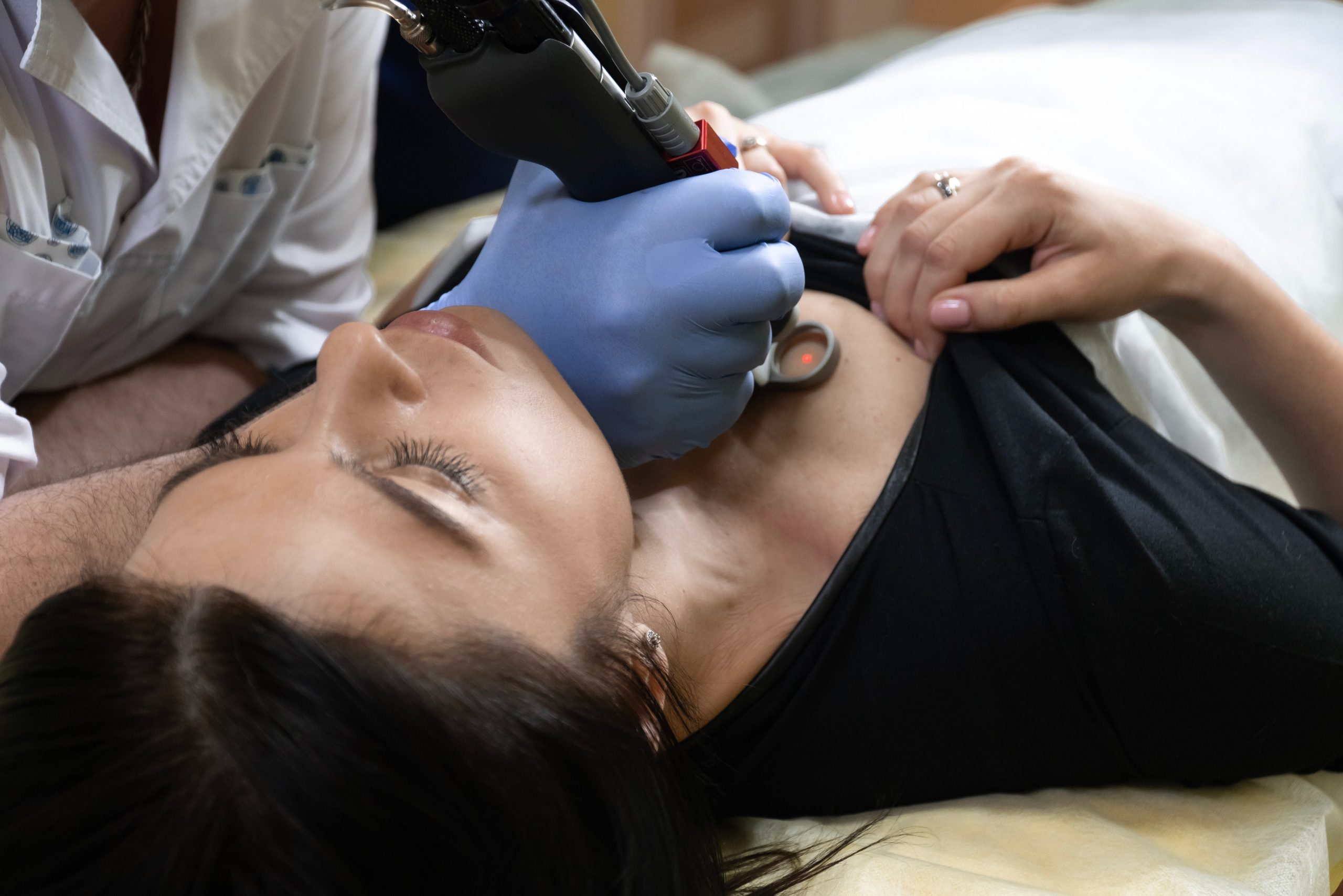
She is a pleasant, slightly overweight young woman. I had seen her in the lobby on my way up to the clinic. Her psoriasis is on full display. “An across the room diagnosis”, an older physician had once called it. I inherited her from one of my colleagues, who recently left the practice. She had improved in the last two months on the methotrexate we prescribed. I ask her how she’s tolerating the medication and she says she hates the nausea and diarrhea but is glad her skin is getting better. I tell her that it’s a common side effect which can be reduced significantly if she takes folic acid daily. She says she sometimes forgets with all that’s going on in her life. Her mom is sick and childcare for her two boys has been a nightmare. I tell her to set an alarm on her phone to remember, and she says she can do that. We make some adjustments and plan to see each other in one month to decide if we want to increase her dose.
:max_bytes(150000):strip_icc()/GettyImages-1154030721-974bcd6d70ff4489ba961317f1f3640f.jpg)
The next gentleman has the most impressive keloids I’ve ever seen in my life. The large, shiny scars engulf the back of his head and neck. He takes off his mask and reveals several more on his face. I feel overwhelmed at the Herculean task ahead of me. I begin by asking him how they affect his life. He does not seem too bothered by them. He has had them for years and has resigned himself to the situation. He mostly wants info: what are they, am I doing something to cause them, are they infectious? Information: clear, unbiased, expert information. I can help him with that. We decide to inject a particularly itchy one on his head with some steroid. We will see each other in a month, and if the injections helped, we may try a few more.
The smell hits me first when I walk into the next room. Fetid. I see a man in his 30s sitting in a gown holding gauze in his groin. He has hidradenitis suppurativa, a long term condition that causes painful boils in his groin and buttocks area. He has been flaring for the last week because his medication was denied by the insurance company. He is trying to hold it together, but I can feel the anguish in his voice. He tells me he cannot work in his present state. We decide to inject some of the larger draining nodules with steroid and start him on an anti-inflammatory oral medication. He needs a note signed by the doctor to miss work for a few weeks. I feel no ambivalence about signing it. I tell him I will see him through this flare and we plan to follow up in a month. I know it’s going to be an uphill battle to get him the medication he needs, but I will remember his face when I am fighting with the insurance company.

The last patient is a dark haired woman in her late 20s: a tired-appearing pediatrics resident at a nearby hospital. She is also to the point of tears. She gives me an incredibly clear history of her hair loss. She was diagnosed five years ago with scarring hair loss. She did a series of five months of steroid injections, which helped a lot. It seemed to have quieted down until a month ago when she started her medical residency. The stress and sleeplessness made it come back with a vengeance. She has had to unclog her bathtub drain every other day from all the shedding. Her scalp was so itchy and the other residents shot her disapproving looks when she scratched her head on bedside rounds. I examined her scalp with my portable dermatoscope and saw diffuse areas of balding with an active red border. This was scarring alopecia: once the hair was gone it wasn’t coming back. I looked at her face at eye level from 3 feet away. My trained eye could just barely make out the white of her scalp. She wouldn’t be able to camouflage it for long. I explained to her what was going on. We needed to be aggressive. I wanted to treat her with systemic immune medication. She hated the idea of having to take pills twice a day with all challenges of residency. I told her that if it was my wife or sister, I would want them to do it. I have seen the psychological devastation that female alopecia can cause. She begrudgingly agrees to give it a try. I injected the advancing active border with steroid, and we plan to follow up in a month.
As I leave the clinic, my thoughts race. How awful it must be to live with pus filled boils in your groin? I am the only thing standing between that beautiful young woman and a lifetime of wigs and awkward explanations. I take a breath and feel the warm sun hit my face. I feel immensely privileged to do what I do. Sometimes it takes writing about it to remember why.